
For any of us who have chronic eczema (also called atopic dermatitis) intense itching, skin-oozing and crusting, and the emotional distress that might accompany flare-ups can be very life-disrupting.
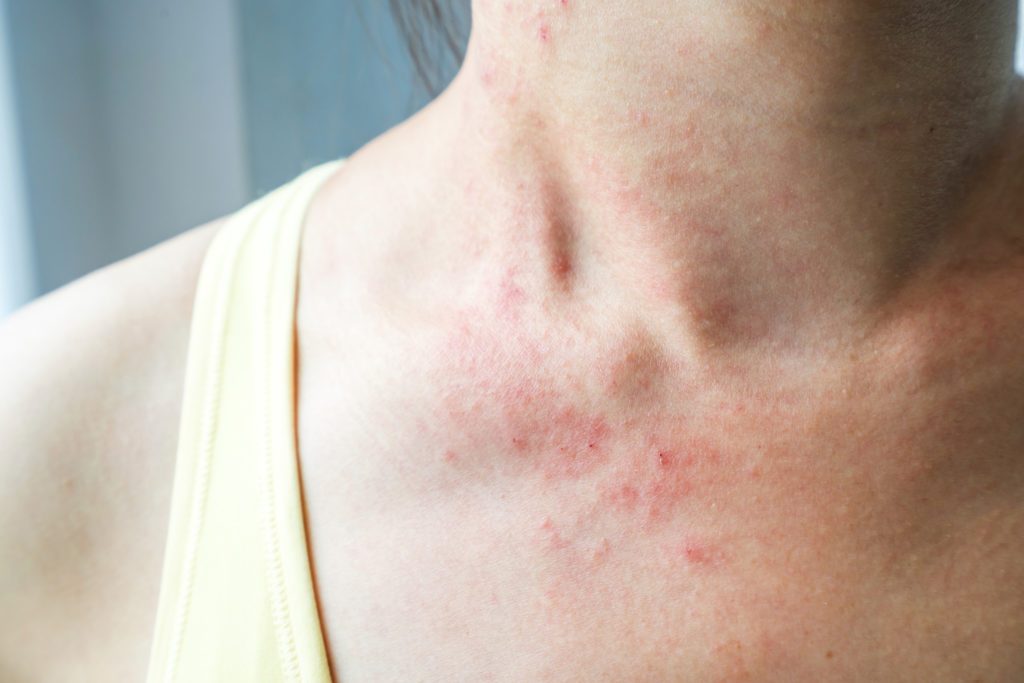
And while eczema often begins when we’re babies, some of us might be ‘lucky’ and symptoms will diminish with age. Still, others might only experience their first bout of eczema in adulthood, leaving sufferers exasperated and asking: Why, what’s causing this?
In short, eczema tends to run in families that have allergies, but eczema also involves an overactive immune system. “Why” this happens isn’t fully understood. What is known is that our immune systems mount an inflammatory response when one isn’t needed.
What is an inflammatory response?
The inflammatory response is the built-in way our immune systems protect us from injury or infection. We can see it in action when we watch a twisted ankle swell and eventually heal or a skin injury scab over and diminish.
The difference with eczema is that there’s no known injury or harmful germ present to trigger the inflammatory response. It’s as if the immune system is left in the “ON” position all the time.
As you probably know, our immune systems are very complex. Some of the system’s “soldiers” act like whistleblowers, calling in many other kinds of specialized troops. And it’s all this action that results in the redness, heat, and itchiness that makes us scratch, sometimes to the point where we might injure the topmost layer of the skin, making the itch-scratch cycle worsen.

Maybe you’ve used a corticosteroid cream or ointments and have had relief? Possibly an antihistamine has helped tone down the inflammatory response? Most of us have had experience with both, but sometimes neither is enough to eliminate intense suffering.
Your family doctor, dermatologist or pharmacist could help you learn about other options to help manage this skin disorder that has affected humans since ancient times.


